In this scenario, the total charges are
for an office visit and an x-ray. The primary insurance paid a portion of the
office visit and the x-ray charge. The EOMB indicated adjustments for exceeding
the fee schedule maximum allowable. The remainder is the patient
responsibility.
Example:
|
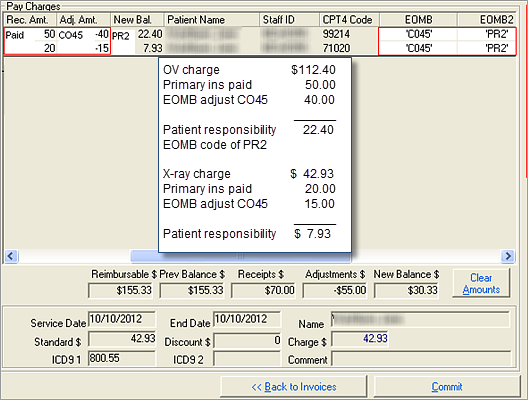
Office Visit:
- Total OV charge: $112.40
- Primary insurance paid: $50.00
- Adjustment: EOMB CO45 - Charge
Exceeds Fee Schedule Maximum Allowable by $40.00
- Patient responsible for balance
$22.40
|
X-ray:
- Total x-ray charge: $42.93
- Primary insurance paid: $20.00
- Adjustment: EOMB CO45 - Charge
Exceeds Fee Schedule Maximum Allowable by $15.00
- Patient responsible for balance
$7.93
|
The steps below presume that
SYSTOC and
SYSTOC_EDI settings are correct before
EOMB codes are applied. It is also presumed that the primary and secondary
insurance information and the relationship to the subscriber have been
documented, as well as the relationship to the patient if there is an alternate
subscriber.
-
Navigate to
.
-
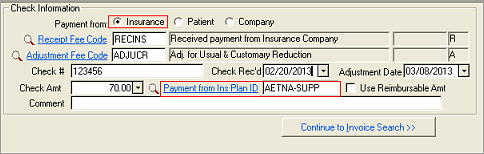
Click the
Insurance
radio button. Browse and select the appropriate insurance plan from the Payment
from Ins Plan ID lookup.
-
Click
Continue to Invoice
Search.
The Search for
Invoices screen displays. Search for the correct invoice using the normal
SYSTOC procedure.
-
Click
Next to Pay
Charges.
The Pay Charges
screen displays.
-
Apply the payments and adjustments.
-
Scroll to the right on the Pay
Charges screen to see the EOMB fields.
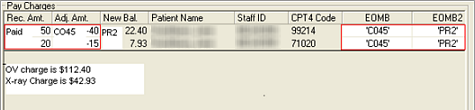
-
Enter the EOMB codes for each line
item.
-
EOMB: Enter the code for the
adjustment or denial.
-
EOMB2: Enter the code for the
person or entity responsible for the remaining balance.
The table below describes
using the two EOMB fields depending on the balance remaining to be paid:
| Line Item has...
|
EOMB Field
|
EOMB2 Field
|
| Remaining
balance after payment and adjustment.
|
Enter the
adjustment or denial reason code.
|
Enter the
appropriate code for person or entity responsible for remaining balance.
|
| Zero balance
after payment and adjustment.
|
Enter the
adjustment or denial reason code.
|
Leave blank.
|
| Zero balance
after payment.
|
Leave blank.
|
Leave blank.
|
The payment, adjustment,
and remaining balance for each line item must equal the total line item charge.
The claim will be rejected if payments and adjustments do not equal the total
charge on the 837 claim file.
-
Click
Commit.
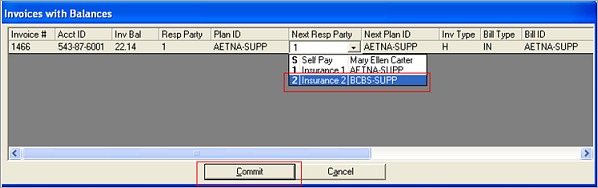
The Invoices
with Balances screen displays.
-
Select the next responsible party
from the drop-down list.
-
Click
Commit to
complete the data entry.
The claim
transmits to the secondary payer when processed.